Centenary celebrations remind us that the First World War, the War to End All Wars, ended 100 years ago. But it did not. It staggered on in much of Europe, it lingered in the broken psyches of soldiers returning home. For some historians, the Great War and the Second World War together form an ‘age of catastrophe’ or even one single war with a long break. The First World War also inaugurated a profound change beneath politics, in a realm largely hidden from journalism or military and political history. The Great War remade the human body itself.
The doctors who identified this new human body saw an organism that organises itself, regulates itself, integrates itself, yet was extremely brittle. It was marked by fragility buried under the skin. It shattered easily, even worked against itself. The great number of injured and maimed bodies enabled doctors to create new kinds of medicine, physiology and psychiatry. In doing so, they also helped to foster a new language of politics and the welfare state.
Hints of this new conception of the body were present before the war, but when tens of thousands of soldiers returned with visible and invisible injuries, disordered hearts and broken psyches, it forced medicine to change too. Triage efforts on the battlefield had been sped up and regularised, and the entire front had become something of a giant medical laboratory for testing ideas and therapies. Many soldiers who, just a few decades earlier, would have died of their wounds now survived them. All of this changed the nature of the relationship between surgeons, physicians and psychiatrists, and patients. With survival, previously unknown pathologies emerged. The way in which medical scientists talked about the patient changed: they now described the patient’s body as an integral whole, and detailed how elaborately it collapses in on itself, system by system, when it is pierced by shrapnel or bullets.
Until about 1900, physiologists discussed the body on a part-by-part basis: the stomach, the lungs, the muscles, the eyes. With the discovery of hormones in 1905 and the first attempts to explain the organisation of the nervous system, organs and regions of the body seemed to merge. Research on them gave a place to work on the processes by which the body regulated itself. Pioneers such as Walter B Cannon at Harvard Medical School and Ernest Starling at University College London explained this regulation on the basis of human evolution. Over millions of years, fluids, reflex arcs and emotions had transformed, helping human bodies to adapt internally by developing more complex responses to external threats.
The war amplified this talk of integration: it distributed and buried wounds deep in the flesh. By 1916, groups of English and American scholars were perplexed by the disparate ways in which patients suffered and died. Many medical scientists created exhaustive case histories of patients – Elmer E Southard in Boston wrote a 1,000-page book with some 600 of them – that couldn’t be readily understood through the panoply of established disorders. An editorial in The Lancet in 1916 lamented that, just as in the fields of eastern France, a ‘no man’s land’ had opened up in medicine.
The complexity of patient symptoms betrayed the need for new ways to think of body-wide effects. Three separate teams raced to understand a condition they eventually named ‘wound shock’. In wound shock, the body reacted to injury with such overwhelming force as to turn even minor blood loss into a system-wide catastrophe. In the UK, the Royal Army Medical Corps established committee after committee, recorded data from the Front, and turned to these new theorists of bodily regulation and integration to help explain the divergence of experiences between patients. One patient, horribly wounded in the stomach, might survive; another, more lightly hurt on the thigh, would die from shock. Why do bodies do that?
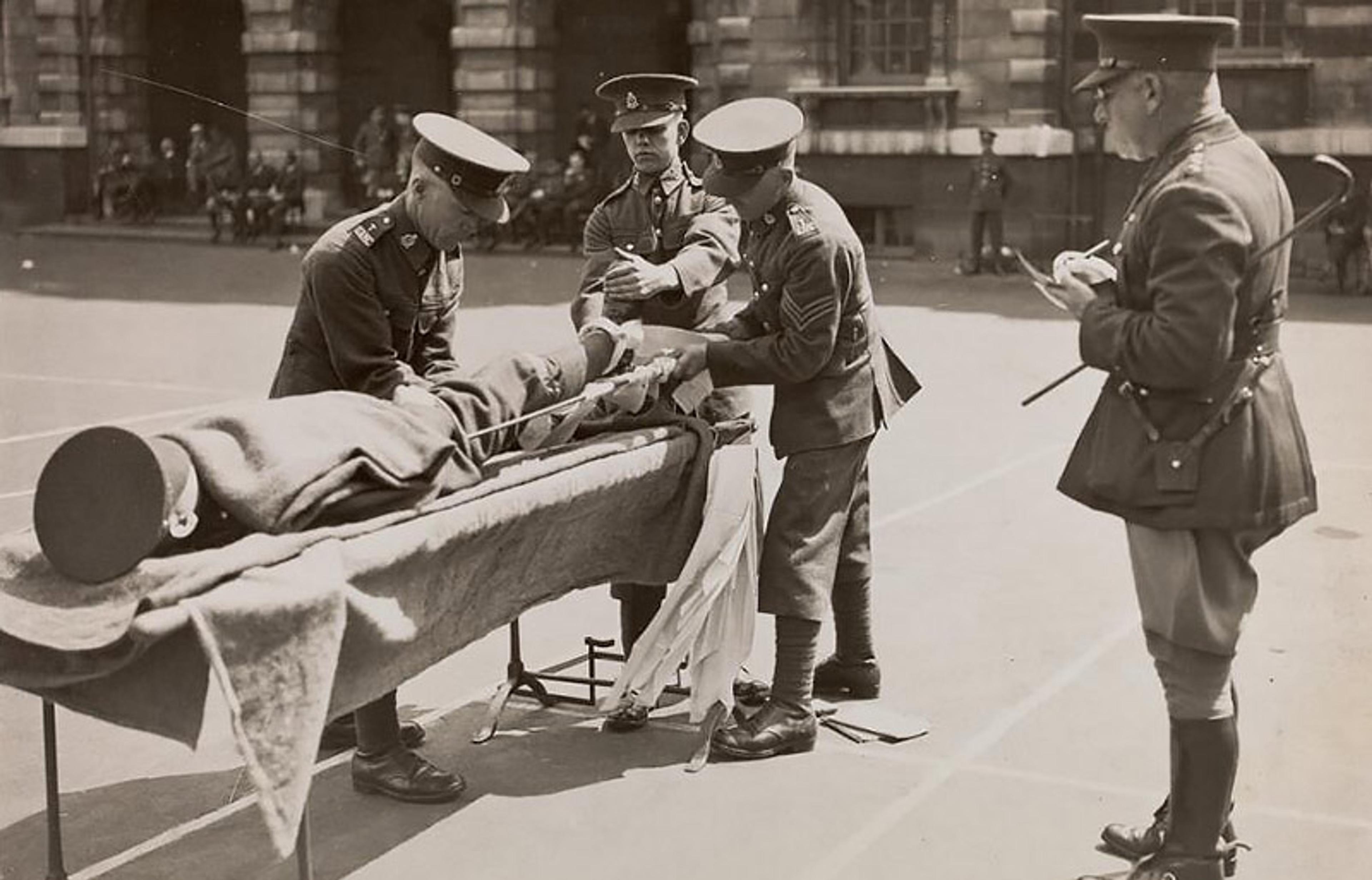
The physiologists offered a straightforward form of care and a complicated theory. Surviving photographs depict soldiers outfitted in splints and covered in three folded blankets. What mattered most were not the splints but the blankets that warmed the injured man. Why? How did this relatively simple form of triage arrest the body’s systemic response to trauma? For the ‘Shock Committee’ in London, blankets were utterly essential to stopping a vicious circle brought on by the injured body, which hid blood in the capillaries to stop it from seeping out of the injured leg. In so doing, the Committee claimed, the body lowered blood pressure, but then, caught in the freezing cold of battle, it watched helpless as its own endocrine, respiratory and circulation systems became trapped while low temperature led to ever-lower pressure. As each system collapsed from lack of blood, they actively helped one another shut down. They were so tightly woven together that they reacted (and failed) together. The discovery of the extent of system integration changed the question; did bodily systems work in concert because any disruption could lead them to break apart and disintegrate?
Neurologists recognised how new relationships formed in and around the bodies of these men
Meanwhile, German and British neurologists asked a similar question about brain injuries: how do you ‘rehabilitate’ a soldier who has barely survived, lost most of his sense of self, can do concrete tasks but can’t calculate or abstract from them, can’t imagine a future? Why can two soldiers with nearly identical brain injuries exhibit such different behaviours? The neurologists Kurt Goldstein in Frankfurt and Henry Head in London (editor, appropriately, of the journal Brain) threw out a century of aphasia research by declaring that what mattered more than the injured lesion was the way that the patient’s brain compensated for its loss. Neurologists had forced their patients onto ‘Procrustean beds’ of theory, rather than looking at them, trying out new ideas with them over and over, until they found out how to make each better.

Different patients compensated differently, and exhibited unpredictable improvement. Their limited capacities might be ordered into a new self. As with shock patients, each brain-injury case was different – each suffered as an individual, each had to be approached as such by medical evaluation. What remained so interesting, troubling and essential was the tendency towards body reintegration that remained unpredictable and dissimilar between individuals. Compensation or self-integration, the capacity of a body to absorb different forms of injury and harm, to work around them, to recalibrate the relationship to an external social environment and to the internal environment of a body’s working physiology, proved crucial. The pursuit of rehabilitation compelled neurologists such as Goldstein to recognise how new relationships formed in and around the bodies of these men. Integration meant that these patients, mostly young men, would change and adapt, or they would not and, very often, die.
The French surgeon René Leriche declared in 1939 that some patients needed a ‘surgery of pain’ to alleviate or alter specific pains that debilitated them because of their responses to past injury. Leriche shared his acute disappointment with medical care in his time, his conviction that patients’ pain had not been addressed:
I am convinced that, almost always, those who suffer suffer quite as much as they say they do, and that, if we assess their pain with the degree of attention which it deserves, they suffer indeed, more than we would imagine. There is only one pain that is easy to bear: it is the pain of others.
The feeling that suffering was always original had spread quickly. ‘How astonishing,’ wrote Virginia Woolf in the essay ‘On Being Ill’ (1926), ‘when the lights of health go down, the undiscovered countries that are then disclosed.’ Psychiatrists – including Sigmund Freud most famously and, even more so, W H R Rivers – charged into these undiscovered countries, blending this individualised patient with anthropological research and physiology into new kinds of psychoanalysis. For her part, Woolf lamented that literature obsessed over the mind, but ‘all day, all night the body intervenes; blunts or sharpens, colours or discolours … The creature within … cannot separate off from the body like the sheath of a knife or the pod of a pea for a single instant.’ She wrote of the unending domination of ‘heat and cold, comfort and discomfort, hunger and satisfaction, health and illness, until there comes the inevitable catastrophe; the body smashes itself to smithereens, and the soul (it is said) escapes’.
While so well-ordered when healthy, bodies were always on the verge of implosion. For years following the war, scientists and doctors theorised about how to reconcile collapse with the mechanisms of bodily stability. Goldstein developed a theory of health, injury and catastrophe: the brain-injured patient needed to be treated closely for years, even decades, maintained within a restricted environment where she could manage life without abstractions, and avoid deep anxiety and ‘catastrophic’ situations. The English pharmacologist Henry Dale showed how histamine, though natural and useful to the organism, can also poison it. Dale claimed that his discovery served as a model of how our bodies both protect and damage themselves. A decade after the war ended, Cannon established the influential theory of homeostasis. To explain why our bodies live comfortably even though they ‘are made of extraordinarily unstable material’, he outlined the complex systems that, within very strict limits, held fast this material. Only these systems could ward off disaster. Medicine now had to prize this complexity, and it had to discover, whether deep within a body or in the overall behaviour of the patient, how these systems and their integration expressed individual patient stories.
In its broad outline, this idea of each patient being an individual survives to our day. We expect that our doctors treat our maladies as wholly our own, each patient original, different from every other patient. We demand that they understand the complex physical systems that make up our bodies but that they also hear and heal us for ourselves. For 19th-century medicine, patients had been more alike than different. The guiding idea of medicine then was to establish laws, build up the body, like a machine, out of its component parts, and cure it by removing any disruption. After the First World War, integration ruled. Medical practice changed to follow a more humanistic course, in which the pain of a patient presents profound disarray that undermines her selfhood and disrupts her life.
Many prominent scientists in the 1920s became socialists: Rivers ran for office with the Labour Party in the UK; Cannon advocated for the New Deal in the US; Goldstein was tortured by the Nazis for advocating on behalf of the Union of Socialist Physicians. Many expressed support for Soviet medicine because they believed that individualism required social welfare. They did not think in liberal mottos devised in the 19th century, nor in racial or evolutionist terms. What, after all, does the grandeur of evolution explain about the sufferer directly confronting the physician? On the contrary: in society as in individuals, only a properly integrated body could guarantee healthy personhood. Yet it is a terrible guarantor, fragile and capricious. The doctor’s role was clear: help the body persevere. By the 1930s, psychiatrists too, from Alexander Luria in Moscow to Karl Lashley in Chicago to Carl G Jung in Zurich were speaking of ‘the integration of the individual personality’ as the key question of psychiatric care.
The new understanding of medicine as a challenge to preserve and balance a delicate natural equilibrium quickly made its influence felt in politics, for example by reviving the ancient ‘body politic’ metaphor. By 1920, policymakers, economists and sociologists found integration to be a choice metaphor for modelling society and the international order. In 1918, the English political theorist Leonard Hobhouse began The Metaphysical Theory of the State with such a new ‘body politic’ analogy:
Just as in the physical body it is the ailment that interests us, while the healthy processes go on without our being aware of them, so a society in which everything is working smoothly and in accordance with the accepted opinion of what is right and proper raises no question for its own members.
To be ‘healed’, Europe needed to be better integrated. John M Keynes used this language on integration and instability to open The Economic Consequences of the Peace (1919), to highlight the ‘unstable, complicated, unreliable, temporary nature of the economic organisation’ of western Europe. The authors of the Treaty of Versailles, he went on, had fooled themselves into ignoring this ‘sandy and false foundation’, and now the Treaty would ‘impair yet further, when it might have restored, the delicate, complicated organisation, already shaken and broken by war’.
Keynes’s thoughts about instability and complicated organisation, about having ‘margin in hand’, staged the life of European societies as relying on economic organisation. He treated political hopes and goals as derivative, and regretted the capacity of economic disorganisation to complete the ruin initiated by the system’s wartime disarrangement. Other economists were more explicit – Wilhelm Röpke spoke of hormones and vitamins of the economy in International Economic Disintegration (1942). Social scientists such as Marcel Mauss, Talcott Parsons, Bronisław Malinowski and Claude Lévi-Strauss also used the idea of the integrated, fragile body in their own pursuits.
The individual patient gave way to the demand for generalisability and replicability between subjects
Physiologists revelled in the attention: Cannon mused in 1940 that, just like the human body in conditions of extreme stress, once mobilised, the body politic would be ‘unified, integrated, and for one purpose: self-preservation’. Human freedom, he concluded, was a matter not of efficiency but of a security that allowed for leeway, for a ‘margin of safety’. The American historian Lewis Mumford, in 1944, recuperated this model of bodily health in the face of ‘changes of circumstance’ to describe the human condition and defend US liberal power. After 1945, the doctors’ defence of a wounded, collapsing individual was gladly co-opted by a muscular Cold War politics that anguished about Western fragility in the face of a supposed Soviet monolith.
The gradual establishment of welfare states in Europe also pursued a version of this medical ideal: not only treatment for as many as possible, but a recognition that every patient will walk a somewhat different path through the welfare state. In Britain, the Beveridge Report of 1942 proposed to use a comprehensive social-insurance system to fight against social ills – the ‘five giants’ of ‘Want …, Disease, Ignorance, Squalor and Idleness’. This required, Beveridge wrote, a new alliance of the state and the individual where each cared for the other’s body. The state promised care and security in exchange for service, and it freed up individuals to ‘build upon it’. Still, in medical thought as in healthcare, the individual patient gave way to the demand for generalisability and replicability between subjects. By the 1970s, the welfare states that physiologists had dreamt would create individualised healthcare were routinely criticised for standardising it instead. Antimedicine advocates, revolutionary antipsychiatrists and neoliberal ideologues all objected that the welfare state was denying the patient the care she deserved, and compared that patient to those injured in war or interned in concentration camps. Several quoted the same First World War generation of physicians – Goldstein, Cannon, Starling – against the welfare state they had helped develop.
It is difficult not to hear echoes of this past today. Integrative medicine continues to push for broader conceptualisations of the whole body in medical practice. Personalised medicine uses medical genetics, gene therapy and predictive pharmacotherapy to shape treatment and prevention around a particularised, neoliberal picture of the patient that supposedly anticipates and guides her destiny. Physical and occupational therapy expend hefty amounts of conceptual and clinical labour to help the individual reconcile her cognitive and physical realities with the demands of her world. The welfare state that tends toward the widest possible inclusion of citizens in its medical schemes clashes ever more intensely with the realities of the medical marketplace, the demand for choice, and the urgencies of individual care and healing.
Meanwhile, patients rely increasingly on online searches and apps that promote a rapid, comforting, but utterly depersonalising self-diagnosis. But perhaps most notable is the gossamer that threads together the aftereffects of injuries from the First World War to the present. Limb loss, permanent disability, traumatic brain injuries, the behavioural changes associated with them and the challenges of reintegration into society after violent injury all remain as critical now (from Sana’a and Aleppo to Chicago) as ever. By the end of the First World War, medicine had transformed the terms by which we understand the human body by declaring it a self-integrating brittle entity. Today we ask what directions this understanding can still take.






