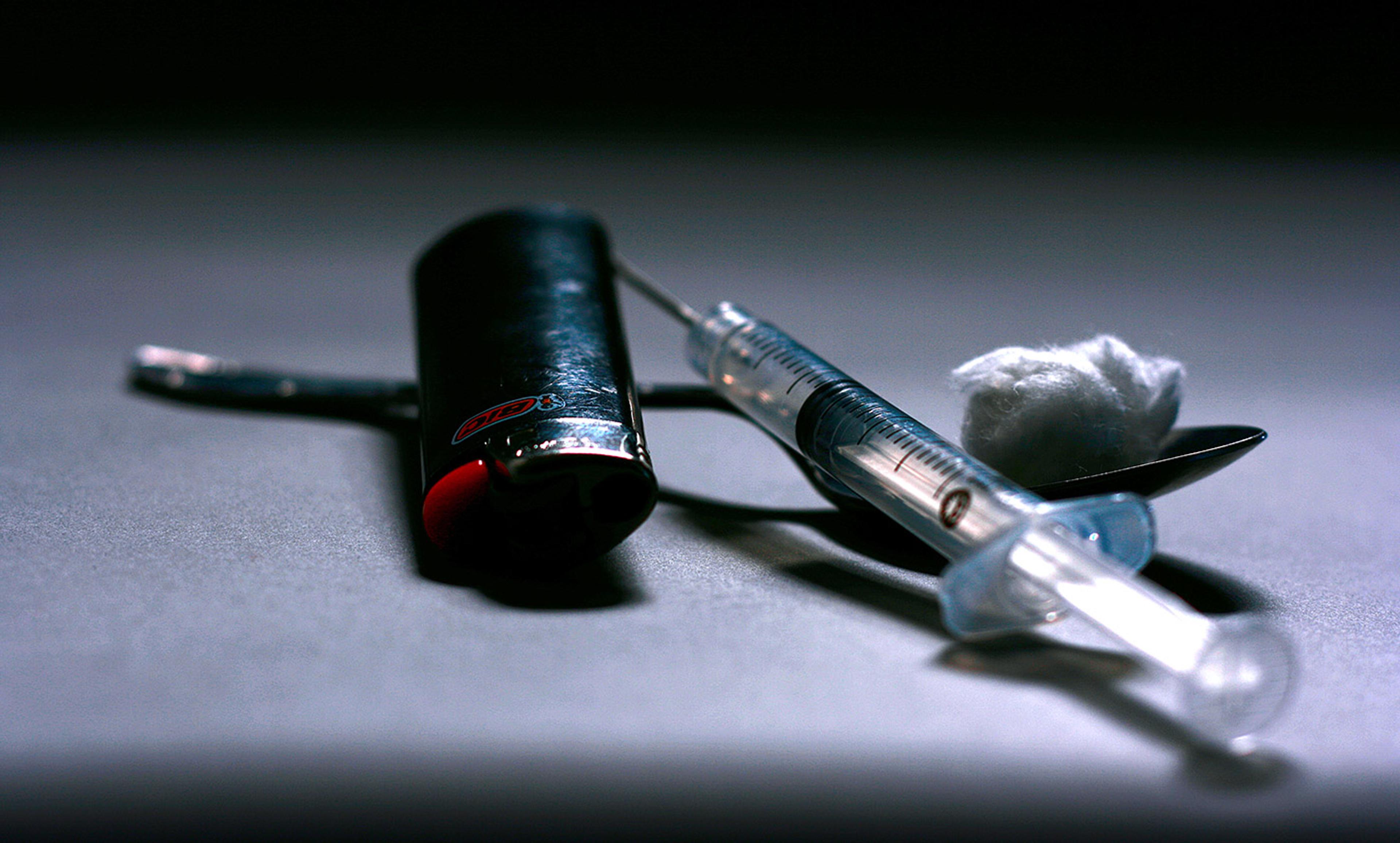
Karen, a heroin addict, trying to save a fellow addict who has overdosed, New York, October 1964. Photo by Bill Eppridge/The LIFE Picture Collection
Heroin, like other opiates, depresses activity in the brain centre that controls breathing. Sometimes, this effect is so profound that the drug user dies, and becomes yet another overdose casualty. Some of these victims die because they took too much of the drug. Others die following self-administration of a dose that appears much too small to be lethal, but why? This is the heroin overdose mystery, and it has been known for more than half a century.
There was a heroin crisis in New York City in the 1960s, with overdose deaths increasing each year of the decade. There were almost 1,000 overdose victims in New York City in 1969, about as many as in 2015. The then chief medical examiner of New York, Milton Helpern, together with his deputy chief, Michael Baden, investigated these deaths. They discovered that many died, not from a true pharmacological overdose, but even when, on the day prior, the victim had administered a comparable dose with no ill effects. Helpern, Baden and colleagues noted that, while it is common for several users to take drugs from the same batch, only rarely does more than one user suffer a life-threatening reaction. They examined heroin packages and used syringes found near dead addicts, and tissue surrounding the sites of fatal injections, and found that victims typically self-administered a normal, usually non-fatal dose of heroin. In 1972, Helpern concluded that ‘there does not appear to be a quantitative correlation between the acute fulminating lethal effect and the amount of heroin taken’.
It was a science journalist, Edward Brecher, who first applied the term ‘overdose mystery’ when he evaluated Helpern’s data for Consumer Reports. Brecher concluded that ‘overdose’ was a misnomer. ‘These deaths are, if anything, associated with “underdose” rather than overdose,’ he wrote.
Subsequently, independent evaluations of heroin overdoses in New York City, Washington, DC, Detroit, and various cities in Germany and Hungary all confirmed the phenomenon – addicts often die after self-administering an amount of heroin that should not kill them.
Most scholarly articles concerning heroin overdose don’t mention the mystery; it is simply assumed that the victim died because he or she administered too much opiate. Even when the mystery is addressed, the explanations are wanting. For example, some have suggested that deaths seen after self-administration of a usually non-lethal dose of heroin result from an allergic-type reaction to additives, such as quinine, sometimes used to bulk up its street package. This interpretation has been discredited.
Others have noted that the effect of a small dose of heroin is greatly enhanced if the addict administers other depressant drugs (such as alcohol) with heroin. Although some cases of overdose can result from such drug interactions, many cases do not.
Some have suggested that the addict might overdose following a period of abstinence, either self-initiated or caused by imprisonment. Thus, tolerance that accumulated during a prolonged period of drug use, and which would be expected to protect the addict from the lethal effect of the drug, could dissipate during the drug-free period. If the addict goes back to his or her usual, pre-abstinence routine, the formerly well-tolerated dose could now be lethal.
But there are many demonstrations that opiate tolerance typically does not substantially dissipate merely with the passage of time. One piece of evidence comes from the addict’s hair, which carries a record of drug use. Many drugs, and drug metabolites, diffuse from the bloodstream into the growing hair shaft; thus, researchers can reconstruct this pharmacological record, including periods of abstinence, using ‘segmental hair analysis’. In a study that analysed the hair of 28 recently deceased heroin-overdose victims in Stockholm, there was no evidence that they had been abstinent prior to death.
A surprising solution to the overdose mystery has been provided by the testimony of addicts who overdosed, then survived to tell the tale. (Overdose is survivable if the antidote, an opiate antagonist, such as naloxone, is administered in a timely manner.) What do these survivors say was special about their experience? In independent studies, in New Jersey and in Spain, most overdose survivors said that they’d administered heroin in a novel or unusual environment – a place where they had not previously administered heroin.
One typical example is the New Jersey survivor who used heroin with others in his living room, following a wedding party. Although he’d used heroin for about 10 years, he’d never before taken heroin in that room or in such a large group.
Similarly, cancer patients receiving medically prescribed opiates for pain relief can suffer an overdose when the drug is administered in novel circumstances. For example, a patient, ‘NE’, with advanced pancreatic cancer was receiving palliative care at home, and had a morphine injection four times per day. Either one of his two sons injected the opiate following procedures specified by the physician. Typically, the preparation of the injection was observed by both sons to ensure accuracy, a regimen that had been ongoing for four weeks.
NE’s condition was such that he stayed in his bedroom, which was dimly lit and contained hospital-type apparatus, and the morphine had always been injected in this environment. For some reason, on the day of the overdose, NE dragged himself to the brightly lit living room. When discovered there by one of his sons, NE appeared to be in considerable pain. Because it was the scheduled time, the son injected the morphine while NE was in the living room, where he’d never previously received the drug. NE suffered an overdose and died. The only feature that distinguished the circumstances of this final, lethal morphine injection from the prior, approximately 100, non-lethal injections would appear to be the novelty of the injection environment.
Case studies suggest an increased risk in an unusual environment, but proof requires an experiment. This experiment cannot ethically be done with people but it has been done with rats and mice. In three independent experiments, conducted at different times, in different laboratories, in different countries, using different drugs, two groups of animals were administered either heroin, pentobarbital or alcohol on a number of occasions. In a final session, one group received the drug in the same environment as prior administrations; another group received it in a novel environment. The consistent finding was that mortality was significantly higher in animals receiving the final dose in an alternative place. In an experiment with heroin, for example, mortality was twice as high in rats receiving their last dose under unusual circumstances.
The findings are bolstered by 40 years of published experiments with many drugs, including caffeine, nicotine and alcohol, showing that effects are augmented when the drugs are taken in a different environment. The drug-taker, who has become tolerant to the drug, loses this tolerance if the drug-administration environment is altered.
Many of us have firsthand experience of this. Perhaps you routinely have a pre-dinner cocktail at the end of a busy day. You relax at home and have a martini. You enjoy the ritual, and don’t think that the drink makes you particularly intoxicated. You don’t normally drink at other times of the working day. However, one day you’re lunching with colleagues and, uncharacteristically, order a drink. Much to your surprise, you find that you’re intoxicated, even though your lunchtime drink had about the same alcohol content as your typical pre-dinner martini at home.
Tolerance is impacted by the pairing of drugs with other cues because of Pavlovian learning. Just as the Russian physiologist Ivan Pavlov in the 1890s demonstrated that a dog learns to respond to an arbitrary signal, for instance a buzzer associated with food, with responses such as salivation, animals (including humans) learn to respond to arbitrary signals for a drug by making drug-preparatory responses. These serve to decrease the drug effect, and are an important mechanism of drug tolerance. In short, heroin addicts who can usually tolerate extraordinarily high doses are at risk of overdose if they administer the drug in an environment not previously associated with the drug effect. They simply are not tolerant on the occasion of the overdose.
Each year, 1 to 3 per cent of heroin addicts die from overdose. There were nearly 13,000 heroin overdose deaths in the United States in 2015. There are several reasons why heroin addicts overdose. Some might simply take too much of the drug, especially when the heroin is enriched with even more potent opioids. Others might die because the effect of a usually sub-lethal dose of opiate is enhanced by other, concomitantly administered, depressive drugs, such as alcohol. These traditional risk factors have been extensively publicised. Less widely acknowledged is the risk that addicts face if they administer the drug in contexts that have not, in the past, reliably signalled the drug. When this occurs, victims die because they don’t have a Pavlovian response, and their bodies fail to decrease the pharmacological insult of the drug. If we told addicts about the risk of using heroin in an unusual setting, lives would be saved.