Photo by Kendal/Unsplash
Numerous criticisms of medical science have been articulated in recent years. Some critics argue that spurious disease categories are being invented, and existing disease categories expanded, for the aim of profit. Others say that the benefits of most new drugs are minimal and typically exaggerated by clinical research, and that the harms of these drugs are extensive and typically underestimated by clinical research. Still others point to problems with the research methods themselves, arguing that those once seen as gold standards in clinical research – randomised trials and meta-analyses – are in fact malleable and have been bent to serve the interests of industry rather than patients. Here is how the chief editor of The Lancet medical journal summarised these criticisms in 2015:
Afflicted by studies with small sample sizes, tiny effects, invalid exploratory analyses, and flagrant conflicts of interest, together with an obsession for pursuing fashionable trends of dubious importance, science has taken a turn towards darkness.
These problems arise because of a few structural features of medicine. A prominent one is the profit incentive. The pharmaceutical industry is extremely profitable, and the fantastic financial gains to be made from selling drugs create incentives to engage in some of the practices above. Another prominent feature of medicine is the hope and the expectation of patients that medicine can help them, coupled with the training of physicians to actively intervene, by screening, prescribing, referring or cutting. Another feature is the wildly complex causal basis of many diseases, which hampers the effectiveness of interventions on those diseases – taking antibiotics for a simple bacterial infection is one thing, but taking antidepressants for depression is entirely different. In my book Medical Nihilism (2018), I brought all these arguments together to conclude that the present state of medicine is indeed in disrepair.
How should medicine face these problems? I coined the term ‘gentle medicine’ to describe a number of changes that medicine could enact, with the hope that they would go some way to mitigating those problems. Some aspects of gentle medicine could involve small modifications to routine practice and present policy, while others could be more revisionary.
Let’s start with clinical practice. Physicians could be less interventionist than they currently are. Of course, many physicians and surgeons are already conservative in their therapeutic approach, and my suggestion is that such therapeutic conservatism ought to be more widespread. Similarly, the hopes and expectations of patients should be carefully managed, just as the Canadian physician William Osler (1849-1919) counselled: ‘One of the first duties of the physician is to educate the masses not to take medicine.’ Treatment should, generally, be less aggressive, and more gentle, when feasible.
Another aspect of gentle medicine is how the medical research agenda is determined. Most research resources in medicine belong to industry, and its profit motive contributes to that ‘obsession for pursuing fashionable trends of dubious importance’. It would be great if we had more experimental antibiotics in the research pipeline, and it would be good to have high-quality evidence about the effectiveness of various lifestyle factors in modulating depression (for example). Similarly, it would be good to have a malaria vaccine and treatments for what are sometimes called ‘neglected tropical diseases’, the disease burden of which is massive. The current coronavirus pandemic has displayed how little we know about some very basic but immensely important questions, such as the transmission dynamics of viruses, the influence of masks on mitigating disease transmission, and the kinds of social policies that can effectively flatten epidemic curves. But there is little industry profit to be made pursuing these research programmes. Instead, great profit can be made by developing ‘me-too’ drugs – a new token of a class of drugs for which there already exist multiple tokens. A new selective serotonin reuptake inhibitor (SSRI) could generate great profit for a company, though it would bring little benefit for patients, given that there are already many SSRIs on the market (and, in any case, their demonstrated effect sizes are extremely modest, as I argued in a recent Aeon essay).
A policy-level change, for which some now argue, is to reduce or eliminate the intellectual property protection of medical interventions. This would have several consequences. It would, obviously, mitigate the financial incentives that appear to be corrupting medical science. It would probably also mean that new drugs would be cheaper. Certainly, the antics of people such as Martin Shkreli would be impossible. Would it also mean that there would be less innovative medical research and development? This is a tired argument often raised to defend intellectual property laws. However, it has serious problems. The history of science shows that major scientific revolutions typically occur without such incentives – think of Nicolaus Copernicus, Isaac Newton, Charles Darwin and Albert Einstein. Breakthroughs in medicine are no different. The most important breakthroughs in medical interventions – antibiotics, insulin, the polio vaccine – were developed in social and financial contexts that were completely unlike the context of pharmaceutical profit today. Those breakthroughs were indeed radically effective, unlike most of the blockbusters today.
Another policy-level change would be to take the testing of new pharmaceuticals out of the hands of those who stand to profit from their sale. A number of commentators have argued that there should be independence between the organisation that tests a new medical intervention and the organisation that manufactures and sells that intervention. This could contribute to raising the evidential standards to which we hold medical interventions, so that we can better learn their true benefits and harms.
Returning to the issue of the research agenda, we also need to have more rigorous evidence about gentle medicine itself. We have a mountain of evidence about the benefits and harms of initiating therapy – this is the point of the vast majority of randomised trials today. However, we have barely any rigorous evidence about the effects of terminating therapy. Since part of gentle medicine is a call to be more therapeutically conservative, we ought to have more evidence about the effects of drug discontinuation.
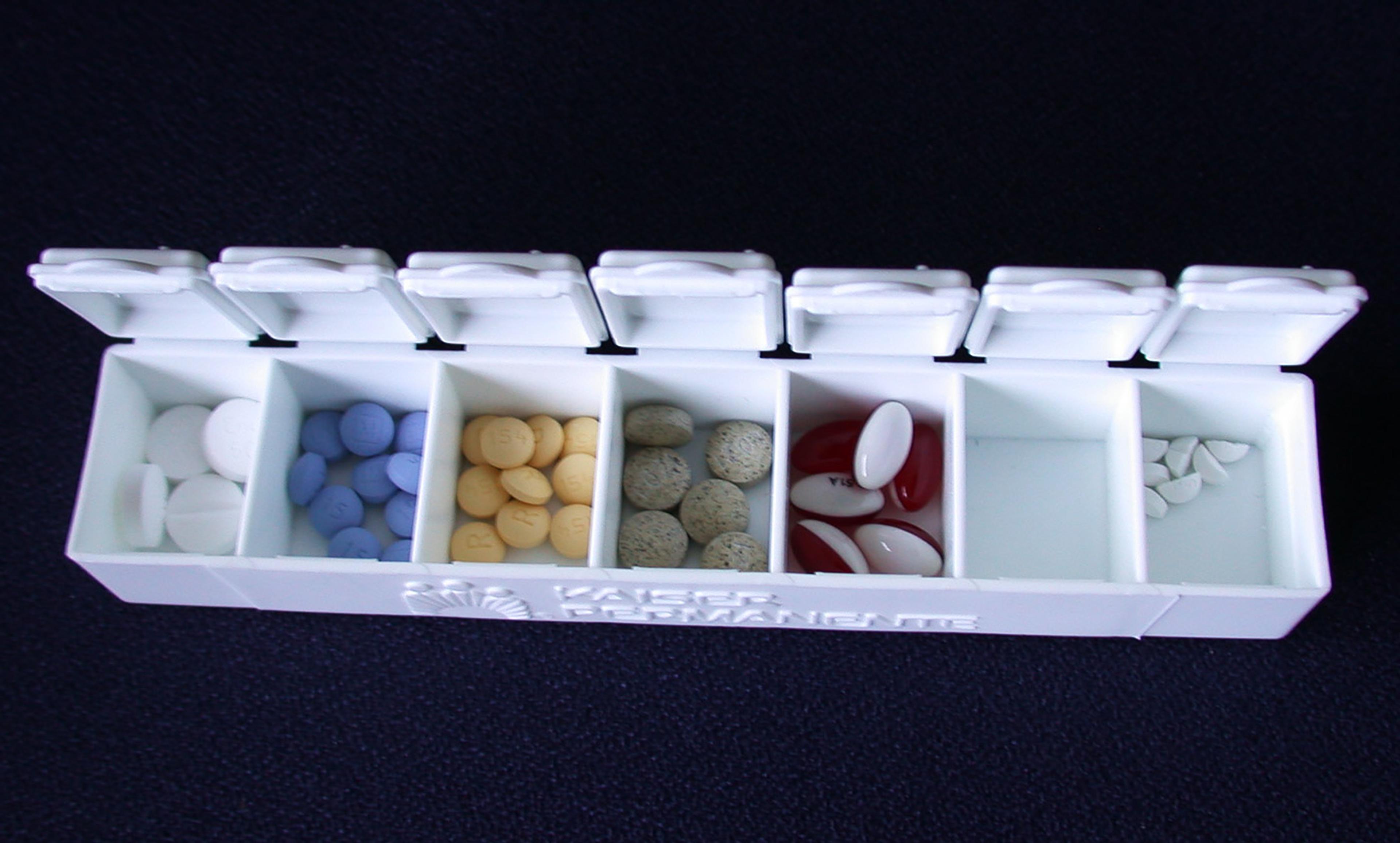
For example, in 2010 researchers in Israel applied a drug discontinuation programme to a group of elderly patients taking an average of 7.7 medications. By strictly following treatment protocols, the researchers withdrew an average of 4.4 medications per patient. Of these, only six drugs (2 per cent) were re-administered due to symptom recurrence. No harms were observed during the drug discontinuations, and 88 per cent of the patients reported feeling healthier. We need much more evidence like this, and of higher quality (randomised, blinded).
Gentle medicine doesn’t mean easy medicine. We might learn that regular exercise and healthy diets are more effective than many pharmaceuticals for a wide range of diseases, but regular exercise and healthy eating are not easy. Perhaps the most important health-preserving intervention during the present coronavirus pandemic is ‘social distancing’, which is completely non-medical (insofar as it doesn’t involve medical professionals or medical treatments), though social distancing requires significant personal and social costs.
In short, as a response to the many problems in medicine today, gentle medicine suggests changes to clinical practice, the medical research agenda, and policies pertaining to regulation and intellectual property.