In a corner of my dad’s cottage in Somerset there is a chest-high stack of photo albums that belonged to my stepmother, Meg. Some of the photographs are holiday snaps and pictures of family, but the majority are of animals and plants. She photographed them wherever she went: during trips around the British Isles and Europe, on the voyage she made to the Galápagos Islands in the 1990s and, most of all, in the cottage’s surroundings. The night-time photographs she took of a family of badgers eating food scraps on the patio at the back of the cottage still hang in its kitchen, as does the picture of a huge comma butterfly resting in sunlight on the ripening cheek of an apple, hanging on its tree.

Born in 1944, Meg trained as a zoologist and spent more than half her adult life working as a field scientist, including a three-year stint on the banks of a chilly Scottish estuary, painstakingly monitoring its population of shelducks. Like the best scientists, she was a passionate witness of the natural world, captivated by its miracles but committed to the pursuit of honesty and clear vision, even when that meant accepting a theory hadn’t panned out or that life had taken a disappointing turn. She carried these convictions over into her second career as a writer, remaining determined in the stories she told that sentiment and reason should exist in equilibrium. I remember the summer afternoon towards the end of her life when she visited my dad and stood in the garden burning her old diaries. She smiled and sighed, as though a great weight were being lifted from her. The longer I live without Meg, and with my memories of her, the more I think I understand her. If she were still here, I like to think we would be friends.
So, when I think about how Meg died, I try to remember how she lived: in search of joy and new beginnings but never in denial of endings.
On the afternoon of 14 May 2010, Meg suffered a massive haemorrhagic stroke in the right temporal lobe of her brain. The following day, when I first saw her, I found her hard to recognise. A breathing tube obscured her mouth and, under the influence of sedation, every inch of her was in gravity’s grip, as though a great hand were pressing her against the bed. Having, at that point, worked with survivors of brain injury for six years, I knew that, if she survived, Meg would almost certainly be significantly changed. Paralysis, language impairment, loss of sensation, memory problems: all of these were on the cards. I wondered how she would cope; how my dad, himself disabled, might care for her. But, over the ensuing few days, I learned these fears were irrelevant.
In a few brain-injury cases each year, a person will neither die nor recover to a recognisable condition. Instead, they will plateau somewhere between coma and waking life, a state of ‘disordered consciousness’, in which the quality of their subjective experience is difficult to discern. Forty-eight hours after her surgery, this was the place in which Meg had come to rest.
I was gripped by the sense that these were the movements of a person on the point of waking
Given the extent of her injuries, the consultant explained, there was scant, if any, chance of further recovery. We were faced with a decision no family wants to make: to insist on treatment that would keep Meg alive in some hope that the doctor was wrong, or to allow the withdrawal of clinically assisted nutrition and hydration and so bring on her death.
When I saw Meg again, a couple of days later, she looked quite different. Her eyes were closed but she was breathing for herself. Where before she had been sallow, she was now pink. Her body was lighter, more alive. Her foot stirred once or twice at the end of the bed. Her hand made a soft circling, as though feeling the texture of the sheets. I was gripped by the sense that these were the movements of a person on the point of waking.
A nurse came in carrying a tray with a dish of water on it. She put the tray down and took a little pink sponge on a stick from the dish.
‘She’s not drinking,’ said the nurse, ‘but this is to stop her mouth getting too dry.’ She offered the sponge to Meg’s lips. At its touch, Meg responded in a way that took me by surprise: she opened her mouth wider and then, as it passed between her teeth, she suddenly bit down and began to chew on it, slowly and then more quickly, with a kind of muscular satisfaction. Her breathing paused as she swallowed, just like a person wide awake, even though her eyes remained closed.
The nurse noticed me staring. ‘That’s just a reflex,’ she said. She took the sponge out of Meg’s mouth and stood to walk away. Meg became still.
I have revisited this moment often in the years since it happened, reflecting on the layers of mystery that were folded into the nurse’s simple statement. Just a reflex. What she meant was that Meg’s movements were not purposeful, not intentional. Meg’s body was here, the nurse was saying, but not her mind. There is a big, simple word for this state that, though neither the nurse nor anyone else used it, hung in the air that day: ‘vegetative’.
When they coined the term ‘vegetative state’ (VS) in 1972, the British neurosurgeon Bryan Jennett and his US colleague Fred Plum were concerned with a new group of patients who were being kept alive by intensive care units opening in Europe and the United States. Like Meg, these patients maintained the essential functions of life independently but did not, Jennett and Plum argued, respond consciously to things going on around them. This condition was distinct from coma, they said, in that comatose people were both asleep and unresponsive, while these new patients were unresponsive despite being biologically awake. They might show behaviours that, to the ‘inexperienced observer or hopeful family’ looked very much like signs of awareness: grasping with their hands, eye movements that appeared to follow objects, withdrawal from noxious smells, chewing and teeth-grinding, swallowing, scratching, weeping, even moaning or crying out. But these were all, as echoed in the language of the nurse caring for Meg, just reflexes.
In seeking a name for this condition, Jennett and Plum considered a number of terms that already existed – coma vigile, apallic syndrome, decorticate state – but concluded that their new one was the ‘most satisfactory’. Their instincts proved right: ‘vegetative state’ was widely adopted in mainstream medicine. Today, it is included in the 11th edition of the World Health Organization’s International Classification of Diseases (2022) and listed on the NHS website as one of the three ‘main disorders of consciousness’ that result from brain injury, along with coma and ‘minimally conscious state’.
It’s the same tradition that’s responsible for racism and misogyny
Yet the term has been causing harm and confusion ever since its conception, upsetting both patients and clinicians, and becoming co-opted for political ends. As the legal advocate Hillary Chua writes: ‘For years, patients in a vegetative state have been at the heart of a right-to-die movement which has influenced perceptions of their social worth and quality of life.’ In caring for these patients, physicians ‘have tended to make nihilistic decisions like neglecting pain management … or hastening death by prematurely withdrawing life support.’ In his Aeon essay ‘Bring Them Back’ (2016), the bioethicist Joseph Fins calls this ‘a kind of neuronal segregation’ and concludes that, contrary to the fatalism surrounding disorders of consciousness (DoCs), there is now ‘incontrovertible evidence’ that a high percentage of patients diagnosed are vegetative are in fact aware and can be helped.
The diagnostic nomenclature for DoCs is poorly evidenced and dangerous, and it needs overhauling. Of the bad terms involved, ‘vegetative state’ is the worst, and it should be abandoned immediately. It was always nihilistic, designed to make the lives of clinicians easier by helping them dismiss the lives of their patients. It is also unscientific, stemming not from observation but from a violent ideology – a metaphysics that fragments the human being, privileging the mind and neglecting the body. It’s the same tradition that’s responsible for racism and misogyny, and for the perpetuation of extractivism, colonialism and slavery.
Perhaps the earliest antecedent of the vegetative metaphor can be found in the writings of Aristotle, who lived at a time of imperialism in ancient Greece. According to his ‘psychic hierarchy’, plants had only the most basic ‘nutritive’ faculty of soul. They could ‘go on living as long as they are able to take nourishment’ but had ‘no other potentiality’. Animals were distinguished from plants by their possession of the perceptive faculty, those senses that gave them awareness of the world around them. At the top of the hierarchy were those beings with the faculty of intellect ‘such as man and any other creature there may be like him or superior to him.’
Aristotle also saw the faculties as organised hierarchically within the individual, writing that the mind is naturally superior to the body and the rule ‘of the mind and the rational element over the passionate is natural and expedient; whereas the equality of the two or the rule of the inferior is always hurtful.’ This normalised the hierarchy present in Greek society at that time. Free, adult men were the natural rulers by dint of their more developed intellectual faculties, ‘for the slave has no deliberative faculty at all; the woman has, but it is without authority, and the child has, but it is immature.’ A person who lacked reason was ‘a slave by nature’.
The habit of formally dividing the world into the animal, vegetable and mineral ‘kingdoms’ emerged later, in tandem with another wave of imperialism, in 18th-century Europe. As awareness of the world’s biodiversity increased, Carl Linnaeus championed the Systema Naturae (1735), a taxonomic theory strongly influenced by ancient Greek philosophy, which imposed order on an otherwise confusing world and demonstrated a divinely ordained hierarchy of value. As Linnaeus put it in a late edition of the System, of the three grand divisions, ‘the animal kingdom ranks highest in comparative estimation, next the vegetable, and the last and lowest is the mineral kingdom.’
Human value was conferred by intelligence, a faculty he tacitly equated with the ability to acquire knowledge
Race was not a peripheral consideration in the Linnaean natural order but its organising principle: all creatures were of a race, and their race was that which defined their value. And this applied as much among human beings as any other creature. In Linnaeus’s terms, for example, Africans were ‘crafty, indolent, negligent’ and ‘governed by caprice’, while Europeans were ‘gentle, acute, inventive’ and ‘governed by laws’.
Taxonomic and psychic hierarchy also influenced the development of neurology and neuroscience. Drawing directly on Aristotle, the 18th-century anatomist Xavier Bichat divided the human nervous system into the ‘animalic life’, responsible for functions that were ‘purely intellectual’ and the ‘vegetative life’, responsible for life-sustaining activity and that existed ‘only within itself’. For the 19th-century neurologist and anthropologist Paul Broca, human value was conferred by intelligence, a faculty he tacitly equated with the ability and willingness to acquire and communicate knowledge after the European tradition. In this quality, he wrote in On the Phenomena of Hybridity in the Genus Homo (1864), white people were ‘inferior to none’ while ‘Hottentots’ were ‘refractory to education’. Broca perceived any barriers to communication as indictments of consciousness and invitations to clinical nihilism. In his landmark case study of Louis ‘Tan’ Leborgne in 1861, he wrote that:
the study of this unfortunate person, who could not speak and who, being paralysed in the right hand, could not write, presented quite a few difficulties … One can scarcely understand that the patient was able to retain any intelligence at all, and it does not seem probable that one could live very long with this kind of brain.
Linnaeus didn’t include microorganisms in his System but, with growing observational data, by the middle of the 19th century there was agreement that a new kingdom was needed to accommodate them. Their diversity caused a time-consuming dispute over which Greek-derived name was most suitable – protozoa (‘first animals’), protoctista (‘first created beings’) or protista (‘the ones who came first in time’). But as all of these names suggest, the primitive status of microbes wasn’t in doubt. Those involved in the debate habitually referred to them as ‘the lower forms of life’, or ‘the lower organisms’, reiterating their simplicity and so maintaining the accepted moral architecture. The 19th-century biologist John Hogg included a diagram to clarify the hierarchy – a pair of pyramids, one yellow, representing the vegetable kingdom, and one blue, the animal, rising from a shared base that he coloured green to represent the domain of the microbes. The upper portion of each pyramid, he explained, was ‘tinged gradually darker, in order to exhibit the higher or more perfect state’ of each as it rose from its base among the ‘lower creatures’.
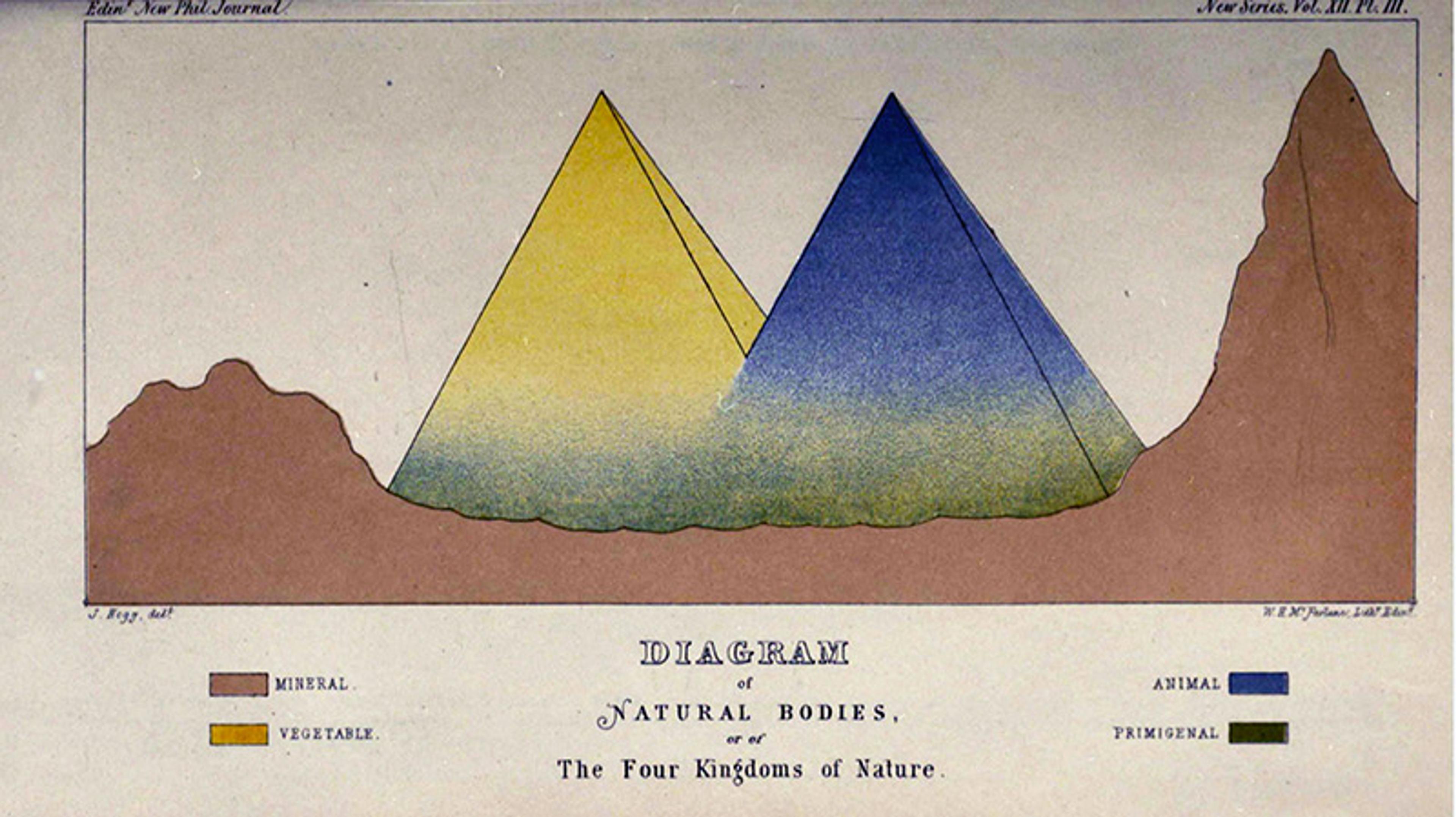
John Hogg’s illustration of the Four Kingdoms of Nature, including a fourth kingdom Regnum Primigenum or Protoctista. Courtesy Wikimedia
The diagnostic paradigm for DoCs follows this same tradition, constructing consciousness vertically and conflating it with virtue. Coma, the lowest rung on this ladder of consciousness, ends when the signs of physiological waking can be detected – with the re-emergence of the sleep-wake cycle, of eye-opening, of diurnal shifts in bodily function. Vegetative state is diagnosed when a person fails to progress from here – ‘awake but unaware’, equipped with ‘mere reflexes’. Traditionally, for a person to be moved to the next category, called minimally conscious state, they need to show at least intermittent signs of ‘purposeful’ responsiveness, for example moving their eyes or a finger when prompted.
When Jennett and Plum created the vegetative state, they acknowledged that their premise could be criticised ‘on the grounds that observation of behaviour is insufficient evidence on which to base a judgment of mental activity’ but concluded that ‘there is no reliable alternative available to the doctor at the bedside, which is where decisions have to be made’. They believed clinicians should go ahead and use the diagnosis for reasons of pragmatism.
Research conducted since the 1990s has repeatedly demonstrated the harm caused by this approach. A review of 40 patients previously diagnosed as vegetative in 1996 showed that 17 were able to demonstrate awareness through deliberate behaviour (eg, eye movements) if they were observed with enough care – suggesting that these 17 had been misdiagnosed due to the inadequacies of the standard clinical observation on which Jennett and Plum felt they could rely.
A proportion of people diagnosed as vegetative can make decisions and respond to complex narratives
Subsequent studies using functional MRI (fMRI) and PET scanning have shown that even some patients with no ability to respond behaviourally can do so through purposeful thinking. By asking patients to imagine different activities that produce MRI activation in different brain areas (eg, playing tennis versus moving around their own home), and then connecting these with ‘yes’ and ‘no’ responses (tennis for ‘yes’, home for ‘no’), the neuroscientist Adrian Owen and colleagues have been able to establish two-way communication with patients. With this method, patients diagnosed as being in a vegetative state have accurately identified previous holiday destinations, recognised their own names and those of loved ones, and demonstrated they know they are in hospital.
More recent research has shown that some VS patients consistently demonstrate the same electroencephalogram readings as uninjured volunteers when asked to imagine performing physical movements. Still others show MRI activation that’s identical to uninjured people when watching Alfred Hitchcock films. Taken together, these studies make it clear that a proportion of people diagnosed as vegetative can comprehend language, follow instructions, sustain and control their own attention, make decisions, and understand and respond to complex narratives. Aside from these ‘functional’ domains, the studies make it hard to doubt that these patients are also having experiences.
This research has also led to greater insight into the real-world impact of the clinical nihilism that accompanies disorders of consciousness in general and the vegetative state in particular. The schoolteacher Kate Bainbridge was one of the earliest subjects enrolled in an fMRI study. Hospitalised with a brain infection in 1997, she was diagnosed as vegetative, and for several months she experienced what sound like terrifying circumstances.
The journalist Roger Highfield interviewed her in 2014, after she had recovered enough to return to her parents’ home and could communicate independently. He wrote:
Sometimes she’d cry out, but the nurses thought it was just a reflex. She felt abandoned and helpless … Kate found physiotherapy scary: nurses never explained what they were doing to her. She was terrified when they removed mucus from her lungs. ‘I can’t tell you how frightening it was, especially suction through the mouth,’ she has written.
To be clear, on this account, the cause of Bainbridge’s suffering was not so much her difficulty in communicating as the fact that her attempts at communication were disregarded by those caring for her. They disregarded both the possibility that she could be suffering and the possibility that she might be trying to communicate with them. And they did this precisely because of her ‘vegetative’ diagnosis.
Of the symptoms of severe brain injury, among the most common are spasticity, paralysis and dysphasia (language impairment). Perhaps unsurprisingly, there is also significant comorbidity between brain injury and post-traumatic stress disorder (PTSD), and research has shown that the functional impacts of stress and anxiety are much worse after brain injury.
Asking a profoundly movement-impaired brain-injury survivor to communicate through outward behaviours, when they are disoriented and in the throes of PTSD and/or significant trauma-induced anxiety, is setting them up to fail.
Diagnosing VS also forecloses explanations for a person’s unresponsiveness at the level of choice. One person I worked with for many years who was significantly movement impaired and had previously been labelled ‘unresponsive’ used a yes-no communication paradigm based on blinking. But he would often disengage or deliberately mess up the system if someone he didn’t like tried to use it with him: there were people he just didn’t want to talk to.
If people are upset by the idea of the ‘vegetative state’, it isn’t because they misunderstand the words
There is no shortage of clinicians who have recognised that ‘vegetative state’ dehumanises their patients. As a group of brain injury specialists based in Cuba and the US put it in 2012: ‘Vegetative state is a pejorative term … We find it difficult to embrace the humanism of a patient who is in an altered state of consciousness when he/she is labelled [in this way].’ Or, as another clinician wrote in 2003: ‘Whatever the technical definition of a word, it may also carry other, sometimes emotive, connotations. “Vegetative” … can so easily be heard as “vegetable”.’ Some commentators have claimed the problem is one of misinterpretation, an unfortunate misunderstanding on the part of the press and public. But ‘vegetative’ was never a neutral clinical description. In their 1972 article, Jennett and Plum were explicit in calling for a name that left no doubt about the condition’s futility:
The word vegetative itself is not obscure: vegetate is defined in the Oxford English Dictionary as ‘to live a merely physical life, devoid of intellectual activity or social intercourse’ (1740) and vegetative is used to describe ‘an organic body capable of growth and development but devoid of sensation and thought’ (1764). It suggests even to the layman a limited and primitive responsiveness to external stimuli … In our view the essential component of this syndrome is the absence of any adaptive response to the external environment, the absence of any evidence of a functioning mind.
Of the 14 other definitions of vegetative offered by the OED today, 10 refer to plants, vegetables or botany, five use the word ‘basic’ or ‘primitive’, and one is an insult, referring to the ‘monotonous, dull; inactive, unchallenging’ nature of certain human lives. If people are upset by the idea of the ‘vegetative state’, it isn’t because they misunderstand the words.
People in disorders of consciousness are a vulnerable population being put at greater risk by the diagnoses imposed upon them. The ‘vegetative state’ diagnosis gives doctors the means of defining a patient’s consciousness out of existence, a way of side-stepping difficult decisions and avoiding what Fins in 2005 called the ‘morass’ of more ambiguous diagnoses. In maintaining this diagnostic nomenclature, the medical profession is dismissing patients’ right to appropriate care, and demonstrating that it doesn’t value their lives. As Fins and his colleague James Bernat put it more recently: ‘Where else in medicine would a diagnostic error rate of over 40 per cent be tolerated?’
Counter-narratives have always been available. Even within the colonialist literature of the period in which Jennett and Plum were socialised and trained, there were decent-enough critical efforts. In his detailed study Behaviour of the Lower Organisms (1906), the influential biologist and eugenicist Herbert Jennings made a cautious examination of the idea of microorganisms’ ‘reflexes’, with significant implications for the study of human consciousness. The decision to attribute a given behaviour as ‘reflex’ or ‘conscious’ in origin, he observed, depends only on where the observer draws the line between ‘state’ and ‘structure’. If an organism’s physiological state is included as part of its structure – that is, as part of a fixed and deterministic condition – then all behaviour can be seen as reflex. And the difference between larger and smaller organisms is ‘one of degree, not of kind’. As Jennings put it: ‘The behaviour of Paramecium [a microbe] and the sea urchin is reflex if the behaviour of the dog and of man is reflex.’
The neurologist Kurt Goldstein rejected taxonomic hierarchies more explicitly in his book The Organism (1934), a ‘holistic theory’ of organismic life. He was, he said:
suspicious of attempts to differentiate between ‘higher’ and ‘lower’ animals, or to understand the ‘higher’ in terms of the ‘lower’ … [I]t is assumed that the lower organisms are more easily understood … But are we sure that, in doing so, one does not overlook the very nature of these beings? May they not seem so ‘simple’ to us because, in investigating them, we simplify them artificially and see in them only that which is consistent with such a simplification?
The decision as to whether a given behaviour in an organism was a ‘reflex’ or something more ‘complex’ depended, Goldstein continued, on one’s understanding of the nature of the organism in question – its needs, priorities, motives, ecology. The challenge on this understanding becomes one of our own capacity for patience and for clear-eyed observation.
Beings who don’t communicate as time-poor professionals want would not be assumed to be ‘mindless’
Over the past few decades, the emergence of genomics has upended taxonomic hierarchy in microbiology. Current understanding is that protists, the tiny organisms studied by Jennings and others, are not a natural group at all but a collection of more-or-less unrelated creatures that are neither animals, vegetables nor fungi. Some of them represent antecedents of larger organisms, most don’t. They aren’t evolutionary ‘primitives’, they are our contemporaries and cousins. Meanwhile, research in plant physiology is challenging accepted distinctions between human and vegetable life on questions of consciousness. Using time-lapse photography to film the behaviour of French bean seedlings, the botanist Paco Calvo in 2020 published results that, for him, indicate intent on the part of the plants. The analysis seems to reveal that plants grown in the presence of a support pole grow towards it in a controlled and predictable way – that they are somehow aware of it and deliberately approach it. Even though this behaviour isn’t neurological as it is in animals, Calvo concludes that it is nevertheless deliberate: ‘This isn’t just adaptive behaviour, it’s anticipatory, goal-directed, flexible behaviour.’
Drawing on this and similar research, the philosopher Emanuele Coccia concludes not only that plants have self-identity but that the self is ‘above all, a vegetable’:
To be an ‘I’ we do not need to have a brain, sense organs, eyes, ears, nose. To have an ‘I’ it’s enough to have a living body, and a body whose main characteristic is the fact of being born … [I]f we ask plants to explain to us what an ‘I’ is, their answer is that the ‘I’ is originally and constitutionally decerebrated, without brain, and without organs, but remains the main plastic force of a living body. The ‘I’ is the property of a body (there is no ‘I’ without a body) capable of growing and shaping itself.
What if our medical metaphors came from sources other than the hierarchical tradition? What if, for example, Jennett and Plum had drawn their paradigm from a more open-ended tradition, in line with the revisionist paradigm of vegetative life presented by Coccia; for example, from the work of the 19th-century abstract painter Hilma af Klint? In her notebooks, af Klint frequently wrote observations of the natural world that confounded the assumptions of taxonomic and psychic hierarchy:
Thinking and feeling are united in the solemnity of every stone.
Warmth and feeling bubble within every living plant.
Behind the agility of every animal rests the power of thought.
Perhaps this suggestion seems challenging. I imagine Jennett and Plum would say it makes no sense to draw medical ideas from the work of an artist. When they coined the ‘vegetative state’, they believed they were borrowing it from a reputable medical source – from Bichat, the 18th-century anatomist. But Bichat took it from Aristotle who was no more qualified to come up with medical metaphors than af Klint. Neither of them rigorously tested hypotheses according to the scientific method. They both based their worldviews as much on the existence of a spiritual realm as on the observation of nature.
As an artist, af Klint worked in the self-reflexive tradition of Socrates equally aware of both the mysterious and the known.
If our approach to medicine followed the intellectual humility of Socrates and af Klint instead of the prejudiced certainty of Aristotle and Bichat, we would be forced to admit that we simply don’t know how conscious people in DoCs are – perhaps even that ‘disorders of consciousness’ are impossible to diagnose. Under this tradition, beings who don’t communicate in the way that time-poor professionals want them to would not be assumed to be ‘unaware’, ‘primitive’ or ‘mindless’. Whether they are plants, or microbes in a Petri dish, or persons in states of disordered consciousness – in a tradition of humility, such beings would inspire curiosity and companionship.
In the end it was Meg, herself so far beyond rescue, who came to ours. Some years earlier, she had signed an advance directive, a document stating her desire not to receive treatment in circumstances of catastrophic brain damage. Three days after her stroke, my father gave permission for her life-support to be withdrawn, and she died a few days later. In the years since then, I have worried sometimes that we made the wrong choice. I believe that Meg’s advance directive played the most significant role in our decision-making but I’m sure our own preconceptions about the meaning of disordered consciousness also came into play, and that the attitudes of the hospital staff, not to mention the fatalism of the wider culture, influenced us too.
I’m still troubled by the memory of Meg chewing on that little sponge. She seemed so alive; and yet this behaviour was so unlike her. One reading of the situation is that Meg was in a state of temporary disarray, that she was on a path to recovery, returning to consciousness, perhaps, even as I watched, and that what I had just seen would eventually become no more than a funny story. Another, the one I believe the nurse wanted me to adopt, is that Meg was nowhere in that room, that everything that constituted Meg before had already vanished, and what remained was merely an empty vehicle.
To meet a loved one in disordered consciousness is to see just how much of what you love is flesh and breath
It would make sense to cleave to one or other of these positions. Depending on your inclination, they both offer to resolve the anxiety and dissonance of what was really happening, which was that Meg was undergoing a transformation, the outcome of which was unknowable.
The journey back from coma is, I believe, an object lesson in the nonsense of psychic and taxonomic hierarchy. Consciousness does not live in some dusty garret of the cranium. It follows a winding shadowed path through the forest of the body, it is snagged in every briar, spun and winnowed like the filaments of a fleece, some aspect carried even at the scale of the single cell. A hand shrugs as though in response to some internal quandary, the lips smack jauntily as though in preparation for speech, the throat growls with a note you recognise. And, if you are paying attention, you will see these signals for what they are – indicators that a person cannot be separated from their body. To meet a loved one in disordered consciousness is to see just how much of what you love is flesh and breath.
I think about Meg on the dunes of that Scottish estuary, carefully counting the number of ducklings in the nests each day and taking readings from the weather station up the road. In the book that resulted partly from her research, there is a photograph of her beaming over two orphaned ducklings she hand-reared. The caption describes her as their ‘foster mother’. She was a scientist in the tradition of Socrates and af Klint and Goldstein; led by curiosity about – and companionship with – other beings.

If we can accept the possibility that consciousness is distributed throughout our bodies and the rest of the world, that we ourselves are part-animal, part-vegetable and part-mineral in nature, and that what we call animals, vegetables and minerals are not lesser beings than we are, perhaps then we can begin to undo the violence we have done – are still doing – to each other and to the evolving ecosphere of which we are an inextricable part.